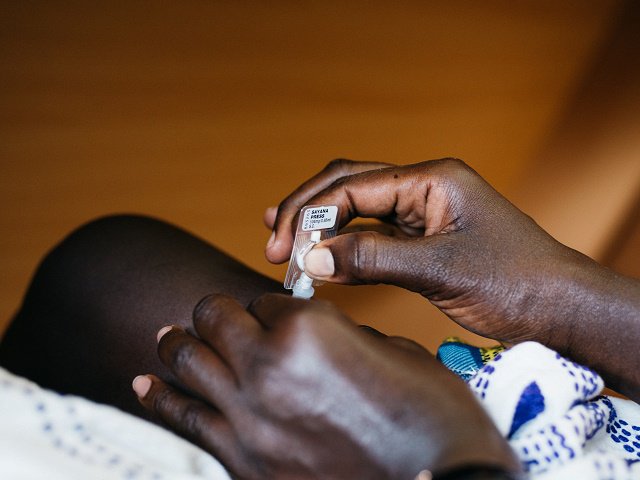
photo courtesy of path.org
Contraceptives reduce the frequency of unplanned pregnancies, unsafe abortions, and death and disability associated with pregnancy and delivery difficulties. To reduce unintended teen pregnancy, family planning services must be both available and accessible to young people given their unique needs and the barriers they face in accessing related care. These obstacles include prohibitive financial costs, lack of transportation, and concerns around confidentiality. Recognizing that young people require care that addresses their needs and helps them overcome barriers, programs that provide family planning and reproductive health services to young people recently have adopted youth-friendly approaches.
We have always employed youth-friendly approaches at Reach a Hand Uganda to guarantee that young people have access to SRHR information and services in order to improve their quality of life. Reach A Hand Uganda partnered with PSI, a non-profit organization, whose goal reimagines how to get quality healthcare to those who need it most by ensuring that all young people have access to the widest range of contraceptive options possible, and that access to services is embraced and advocated for by young people, their health providers, governments, families, and communities. Rethink and redefine how sexual and reproductive health and rights programs are created, administered, measured, and evaluated. Increase adolescent trust in the health-care system and encourage them to utilize contraceptives for the rest of their lives.
Self-care can assist in achieving improved sexual and reproductive health. Self-care is an innovation with the potential to impact many sectors. Diabetics are already using self-care treatments to self-administer insulin and to self-test for HIV. Self-injectable contraceptives can help boost the use of contemporary contraceptives by giving women and young people with an effective and unobtrusive option to fulfill and manage their contraceptive needs, which is good for sexual and reproductive health. Population Services International (PSI) in collaboration with Reach A Hand Uganda introduces a self-injectable contraception, which is a self-inject contraceptive that you inject privately and receive 3 months of safe, effective, and reversible protection from unintended pregnancy. It is 99 % effective, more discreet, and may be readily administered by the consumer anytime and anywhere, closing the gap between access to contraceptive products and services for young people due to many hurdles.
Population Services International (PSI) Uganda teamed with the Pan-African edutainment series Kyaddala, It’s Real to bring the concept of self-injectable contraception into the public as part of their outreach activities. Kyaddala, It’s Real has been weaving in stories that resonate with young people across Uganda and the many gatekeepers they must engage with as they navigate various challenges in their daily lives, from relationships and career guidance to concerns about gender-based violence and unplanned pregnancies, since it launched in October 2019. The first season of the show featured characters suffering sexual assault, pursuing their dreams while juggling huge obligations, dealing with HIV stigma, being pushed into an arranged marriage, and exploring love and sex.
PSI Uganda collaborated with Reach a Hand Uganda (RAHU) to develop the second season of Kyaddala, It’s Real as part of the Delivering Innovation in Self Care (DISC) project. The show, which is aimed at a 15–24-year-old demographic, provides a unique chance to make the self-inject process, including the decision-making stage, genuine and relevant to viewers through the show’s characters and this is because Edutainment, or educational entertainment, has changed the game. From movies to TV shows, entertainment media is increasingly being used to raise awareness and change attitudes about a variety of sensitive topics, such as sexual and reproductive health and rights, and has the potential to provide life-saving information to address some of the world’s most pressing health issues.
According to data from the Guttmacher Institute (2019), sexual and reproductive health services for adolescent women in Uganda are severely lacking. For example, 648,000 Ugandan women aged 15–19 are sexually active but do not wish to have a child in the next two years. However, more than 60% of this group has an unmet need for contemporary contraception, which means they either don’t utilize any kind of contraception or use a traditional technique. Unwanted pregnancies account for over half of all pregnancies among Ugandan women aged 15–19, with an estimated 214,000 unintended pregnancies per year. The vast majority of these pregnancies (88%) occur among teens who do not have access to contemporary contraception (FP 2030). In a country where the fertility rate is 5.4 children per woman, the pressure is on to close the gaps in providing Ugandan women and girls with the tools and information they need to better manage their sexual and reproductive health.
Self-administered contraception may provide more privacy and access to injectable contraception, especially for those who have difficulty getting to clinics. Unmarried young people, in particular, face negative stigma while seeking services and may lack the financial resources to go to clinics for regular reinjection. Self-injection may provide solutions to the unique access challenges that unmarried young people face, such as concerns about privacy and confidentiality stemming from the stigma of contraceptive use and premarital sex; the cost of travel and distance to health facilities for adolescents who lack financial autonomy and find it difficult to travel independently; and inconvenient clinic hours. Despite efforts to improve services for young people in Uganda, there is still a significant shortage of youth-friendly services, with nonjudgmental, supportive front-line health care personnel playing a vital role.
Your Reaction